Setiap orang tua pasti akan suka jika melihat anak terlalu bersih. Mereka beranggapan bahwa kebersihan yang total seperti itu akan membawa dampak baik, khususnya untuk kesehatan. Namun, siapa sangka beberapa penelitian justru menunjukkan bahwa kebiasaan itu kurang baik. Bagaimana bisa dan apa saja alasan dibalik hasil penelitian itu? Korelasi Anak Terlalu Bersih dan Alergi Menurut... Baca Sekarang
- April 26, 2024
 Putri Dian AyuKebiasaan Anak Terlalu Bersih Justru Kurang Baik, Benarkah?Setiap orang tua pasti akan suka jika melihat anak terlalu bersih. Mereka beranggapan bahwa kebersihan yang total seperti itu akan membawa dampak baik, khususnya untuk kesehatan. Namun, siapa sangka beberapa penelitian justru menunjukkan bahwa kebiasaan itu kurang baik. Bagaimana bisa dan apa saja alasan dibalik hasil penelitian itu? Korelasi Anak Terlalu Bersih dan Alergi Menurut...Kesehatan, Lifestyle
Putri Dian AyuKebiasaan Anak Terlalu Bersih Justru Kurang Baik, Benarkah?Setiap orang tua pasti akan suka jika melihat anak terlalu bersih. Mereka beranggapan bahwa kebersihan yang total seperti itu akan membawa dampak baik, khususnya untuk kesehatan. Namun, siapa sangka beberapa penelitian justru menunjukkan bahwa kebiasaan itu kurang baik. Bagaimana bisa dan apa saja alasan dibalik hasil penelitian itu? Korelasi Anak Terlalu Bersih dan Alergi Menurut...Kesehatan, Lifestyle - April 19, 2024
 Hannah Rasyid4 Game MotoGP Terbaik yang Wajib Dimainkan, Seru!Game MotoGP wajib dimainkan apabila Anda adalah penggemar sejati Valentino Rossi, Marc Marquez, Jorge Lorenzo, hingga Daniel Pedrosa. Game ini memberikan Anda pengalaman dan adrenalin layaknya sedang di sirkuit balapan. Terdapat berbagai macam game balap yang bisa Anda coba. Berbagai rekomendasi dalam pembahasan berikut cocok untuk Anda yang ingin merasakan sensasi balapan bersama jagoan balap...Gaming
Hannah Rasyid4 Game MotoGP Terbaik yang Wajib Dimainkan, Seru!Game MotoGP wajib dimainkan apabila Anda adalah penggemar sejati Valentino Rossi, Marc Marquez, Jorge Lorenzo, hingga Daniel Pedrosa. Game ini memberikan Anda pengalaman dan adrenalin layaknya sedang di sirkuit balapan. Terdapat berbagai macam game balap yang bisa Anda coba. Berbagai rekomendasi dalam pembahasan berikut cocok untuk Anda yang ingin merasakan sensasi balapan bersama jagoan balap...Gaming - April 17, 2024
 Renny NurhasanahTeknik Dasar Permainan Olahraga Kriket hingga Cara BermainPermainan olahraga kriket atau cricket merupakan salah satu jenis olahraga musim panas asal Inggris. Di mana sekarang telah dimainkan di seluruh dunia, terutama India, Pakistan, Australia, Kepulauan Karibia, serta Kepulauan Britania. Sejarah olahraga kriket ini mulai diyakini muncul sejak abad ke-13 silam. Di mana pertandingan akan dipimpin oleh dua wasit yang tugasnya menentukan keputusan skor,...Olahraga
Renny NurhasanahTeknik Dasar Permainan Olahraga Kriket hingga Cara BermainPermainan olahraga kriket atau cricket merupakan salah satu jenis olahraga musim panas asal Inggris. Di mana sekarang telah dimainkan di seluruh dunia, terutama India, Pakistan, Australia, Kepulauan Karibia, serta Kepulauan Britania. Sejarah olahraga kriket ini mulai diyakini muncul sejak abad ke-13 silam. Di mana pertandingan akan dipimpin oleh dua wasit yang tugasnya menentukan keputusan skor,...Olahraga - April 15, 2024
 Hannah RasyidRekomendasi Modem Wifi 4G, Gadget Terbaik untuk Internet CepatDi era digital seperti sekarang, memiliki koneksi internet yang cepat dan stabil merupakan hal yang sangat penting, terutama bagi yang bekerja dari rumah (WFH). Salah satu cara mendapatkan koneksi internet cepat adalah dengan gadget terbaik seperti modem WiFi 4G. Modem ini memungkinkan penggunanya untuk terhubung dengan jaringan 4G LTE dan menikmati kecepatan internet secara maksimal,...Teknologi
Hannah RasyidRekomendasi Modem Wifi 4G, Gadget Terbaik untuk Internet CepatDi era digital seperti sekarang, memiliki koneksi internet yang cepat dan stabil merupakan hal yang sangat penting, terutama bagi yang bekerja dari rumah (WFH). Salah satu cara mendapatkan koneksi internet cepat adalah dengan gadget terbaik seperti modem WiFi 4G. Modem ini memungkinkan penggunanya untuk terhubung dengan jaringan 4G LTE dan menikmati kecepatan internet secara maksimal,...Teknologi - April 13, 2024
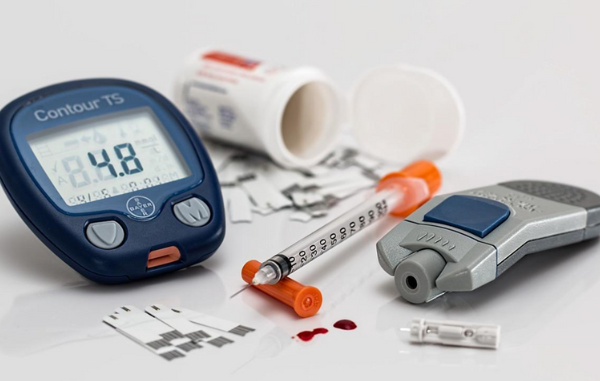
 Renny NurhasanahCara Menjaga Kesehatan Tubuh untuk Penderita DiabetesDiabetes mellitus adalah kondisi kronis yang ditandai dengan kadar glukosa darah yang tinggi karena tubuh tidak dapat menggunakan glukosa secara efektif. Penderita diabetes perlu memperhatikan kesehatan tubuh lebih ekstra supaya kadar gula darah stabil. Sebab jika tidak, maka komplikasi serius akan menghantui penderita diabetes. Untuk itu, ikuti panduan menjaga kesehatan bagi penderita diabetes. Panduan Jaga...Kesehatan
Renny NurhasanahCara Menjaga Kesehatan Tubuh untuk Penderita DiabetesDiabetes mellitus adalah kondisi kronis yang ditandai dengan kadar glukosa darah yang tinggi karena tubuh tidak dapat menggunakan glukosa secara efektif. Penderita diabetes perlu memperhatikan kesehatan tubuh lebih ekstra supaya kadar gula darah stabil. Sebab jika tidak, maka komplikasi serius akan menghantui penderita diabetes. Untuk itu, ikuti panduan menjaga kesehatan bagi penderita diabetes. Panduan Jaga...Kesehatan
Game MotoGP wajib dimainkan apabila Anda adalah penggemar sejati Valentino Rossi, Marc Marquez, Jorge Lorenzo, hingga Daniel Pedrosa. Game ini memberikan Anda pengalaman dan adrenalin layaknya sedang di sirkuit balapan. Terdapat berbagai macam game balap yang bisa Anda coba. Berbagai rekomendasi dalam pembahasan berikut cocok untuk Anda yang ingin merasakan sensasi balapan bersama jagoan balap... Baca Sekarang
Permainan olahraga kriket atau cricket merupakan salah satu jenis olahraga musim panas asal Inggris. Di mana sekarang telah dimainkan di seluruh dunia, terutama India, Pakistan, Australia, Kepulauan Karibia, serta Kepulauan Britania. Sejarah olahraga kriket ini mulai diyakini muncul sejak abad ke-13 silam. Di mana pertandingan akan dipimpin oleh dua wasit yang tugasnya menentukan keputusan skor,... Baca Sekarang
Di era digital seperti sekarang, memiliki koneksi internet yang cepat dan stabil merupakan hal yang sangat penting, terutama bagi yang bekerja dari rumah (WFH). Salah satu cara mendapatkan koneksi internet cepat adalah dengan gadget terbaik seperti modem WiFi 4G. Modem ini memungkinkan penggunanya untuk terhubung dengan jaringan 4G LTE dan menikmati kecepatan internet secara maksimal,... Baca Sekarang
Diabetes mellitus adalah kondisi kronis yang ditandai dengan kadar glukosa darah yang tinggi karena tubuh tidak dapat menggunakan glukosa secara efektif. Penderita diabetes perlu memperhatikan kesehatan tubuh lebih ekstra supaya kadar gula darah stabil. Sebab jika tidak, maka komplikasi serius akan menghantui penderita diabetes. Untuk itu, ikuti panduan menjaga kesehatan bagi penderita diabetes. Panduan Jaga... Baca Sekarang
Sukabumi adalah salah satu kabupaten yang berada di Jawa Barat. Meskipun wilayah ini relatif kecil, tapi menyimpan sederet wisata Indonesia yang memukau. Kota ini berlokasi di antara Gunung Pangrango dan Gunung Gede sehingga tidak heran jika ada banyak jenis wisata menarik yang ditawarkan. Mulai dari wisata bukit, danau, pantai, dan air terjun, bisa Anda temukan... Baca Sekarang
Organisasi ekonomi global di dunia cukup banyak jumlahnya. Keberadaan organisasi tersebut terbentuk berdasarkan kondisi perekonomian antar negara yang saling membutuhkan. Melalui organisasi ekonomi skala global, masalah perekonomian suatu negara dapat diatasi. Sebab, organisasi tersebut akan mempromosikan investasi serta perdagangan internasional negara anggotanya. Jadi, perekonomian di antara negara lebih terintegrasi. Berikut daftarnya! Ini Daftar Organisasi Ekonomi... Baca Sekarang
Ada berbagai macam jenis latihan fisik yang sangat penting untuk dilakukan oleh para pemain sepak bola. Indonesia merupakan salah satu negara yang memang sangat mencintai sepak bola. Hal tersebut bisa tercermin dengan jelas dari banyaknya penonton yang hadir ketika pertandingan-pertandingan sepak bola digelar. Para atlet sepak bola tentu saja harus menjaga kebugaran tubuhnya supaya bisa... Baca Sekarang
UPS (Uninterruptible Power Supply) merupakan gadget terbaik untuk melaksanakan fungsi pengamanan data komputer apabila terjadi mati listrik mendadak. UPS akan berperan sebagai sumber listrik selama durasi tertentu. Ini memungkinkan Anda melakukan backup data dengan efektif. Anda juga masih sempat mematikan komputer dengan normal. Kerusakan komputer pun dapat diminimalkan. Itulah mengapa, penting bagi Anda untuk memiliki... Baca Sekarang
Kehidupan yang panjang dan berkualitas adalah dambaan setiap orang. Hasilnya adalah sosok yang tampak bahagia dan awet muda. Hal itu bisa didapatkan dengan penerapan lifestyle sederhana tapi sehat. Anda bisa menerapkan hal tersebut dengan melakukan kebiasaan kecil dulu lho! Berikut adalah beberapa tips gaya hidup sederhana yang dapat membantu Anda tetap awet muda dan merasa... Baca Sekarang